Dermatophytosis
Issues
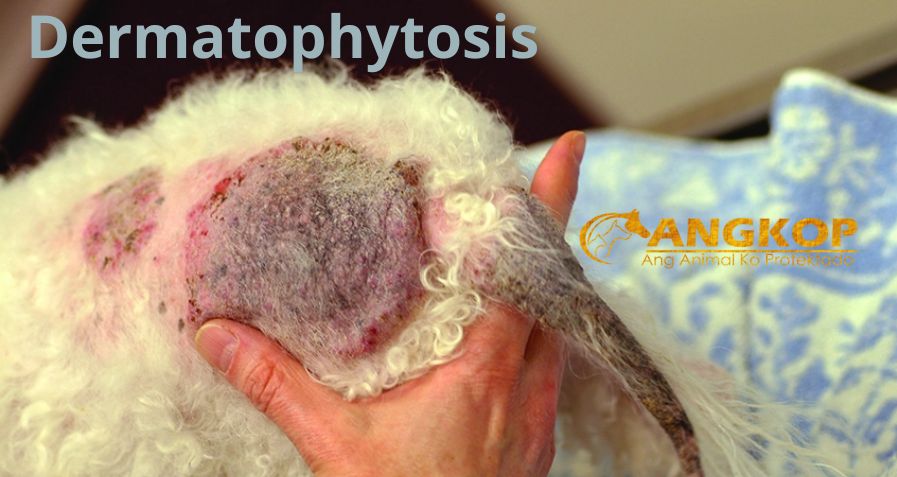
Dermatophytosis
- A cutaneous fungal infection affecting the cornified regions of hair, nails, and occasionally the superficial layers of the skin.
- Microsporum and Trichophyton dermatophytes are most commonly isolated: the majority of cases are caused by Microsporum canis; infection with Trichophyton mentagrophytes, M. gypseum, or M. persicolor also occurs.
- PATHOPHYSIOLOGY
- Dermatophytes—grow in the keratinized layers of hair, nail, and skin; do not thrive in living tissue or persist in the presence of severe inflammation.
- Exposure to or contact with a dermatophyte does not necessarily result in an infection.
- Infection may not result in clinical signs.
- Incubation period from exposure to clinical lesions: approximately 2–4 weeks.
- Infective spores must contact the skin surface and defeat host protective mechanisms (innate immunity, normal flora, sebum, grooming), in order for infection to occur.
- Factors that favor the development of disease: stress, trauma, ectoparasite infestations, and immunosuppression.
- An infected animal may remain as an asymptomatic (inapparent) carrier for a prolonged period of time; some animals never become symptomatic.
SYSTEMS AFFECTED
Skin/Exocrine
INCIDENCE/PREVALENCE
- Lesions may mimic many dermatologic conditions; over-diagnosis is likely common.
- Infection rates (inapparent and clinical) vary widely, depending on the population studied.
- GEOGRAPHIC DISTRIBUTION
- More common in hot, humid climates.
- Incidence of dermatophyte species may vary seasonally and geographically (e.g., northern vs. southern hemisphere, rural vs. urban environment, indoor vs. outdoor housing).
SIGNALMENT
Species
Dog and cat
Breed Predilections
- Cat—more common in longhaired breeds (i.e., Persian and Himalayan)
- Dog: Yorkshire terrier and Manchester terrier
Mean Age and Range
- M. canis is more common in younger animals; other species (associated with rodents or wildlife) seen more often in adults.
- Generalized dermatophytosis in older dogs associated with immunosuppression.
SIGNS
Historical Findings
Previously confirmed infection or exposure to an infected animal or environment (e.g., a cattery) is a useful but not consistent finding.
Physical Examination Findings
- Inapparent carrier state–cats.
- Only consistent finding is extreme variability of clinical signs.
- Classical lesion: slowly expanding circular patch of alopecia with scale.
- Seborrheic or greasy hair coat.
- Papular or pustular eruptions.
CAUSES
Multiple species identified; majority of cases caused by Microsporum canis, Microsporum gypseum, Tricophyton mentagrophytes, and Microsporum persicolor (non-follicular).
RISK FACTORS
- Immunocompromised caused by disease (FeLV, FIV) or by medications (glucocorticoids).
- High population density.
- Poor management practices.
DIAGNOSIS
DIFFERENTIAL DIAGNOSIS
- Staphylococcal folliculitis
- Demodicosis
- Allergic dermatitis
- Pemphigus (especially foliaceus)
- Keratinization defects
DIAGNOSTIC PROCEDURES
Wood’s Lamp Examination
- Can be misleading: only 50% of M. canis isolate fluoresce; most other pathogenic dermatophytes do not fluoresce.
- True positive reaction consists of apple-green fluorescence of the hair shaft.
Microscopic Examination of Hair
- Choose hairs that fluoresce under Wood’s lamp illumination to increase success.
- Hyphae and arthrospores seen invading hair shafts.
Fungal Culture with Identification
- “Gold standard” for diagnosis.
- Choose hairs that fluoresce under Wood’s lamp if possible.
- Sampling methods: Pluck hairs from the periphery of an alopecic area. Brush haircoat with a sterile toothbrush or carpet square (especially inapparent or treated patient.
- Dermatophyte test media—dermatophytes change media color to red during the early growing phase of the culture; saprophytes cause color change after significant colony growth; examine inoculated media daily.
- Fungal colonies are non-pigmented.
- Microscopic examination of the growth for microconidia and macroconidia—necessary to confirm pathogenic dermatophyte and to identify genus and species; helps identify source of infection.
- Positive culture—indicates presence of a dermatophyte; however, organisms may be transient (i.e., geophilic dermatophytes on the feet).
Skin Biopsy
- Not usually required for diagnosis.
- Can be helpful in confirming true invasion and infection, or to diagnose suspicious cases with negative fungal culture.
PATHOLOGIC FINDINGS
- Folliculitis, perifolliculitis, or furunculosis.
- Hyperkeratosis, intraepidermal pustules, and pyogranulomatous reaction patterns may occur.
- Fungal hyphae seen in H&E-stained sections; special stains allow easier visualization of the organism.
TREATMENT
APPROPRIATE HEALTH CARE
- Most animals are treated as outpatients.
- Consider quarantine owing to the infective and zoonotic nature of the disease.
CLIENT EDUCATION
- Many shorthaired cats in a single-cat environment and many dogs will undergo spontaneous remission within 3 months.
- Longhaired animals should be clipped to reduce environmental contamination.
- Decontamination of the environment reduces the risk of false positive fungal cultures which can lead to prolonged treatment and confinement.
- Infective spores are shed into the environment, but do not multiply in the environment; transmission of the disease strictly from a contaminated environment (i.e., no direct contact with an infected animal) is extremely rare.
- Effective disinfectants
- Sodium hypochlorite (0.5%): potential to react with other chemicals to create toxic gases; can be irritating and result in “bleaching” of colors.
- Enilconazole: available as a concentrated spray or fogger; 10-minute contact time is recommended.
- Accelerated hydrogen peroxide: should not be mixed with concentrated sodium hypochlorite products; 10-minute contact time recommended.
- Potassium peroxymonosulfate (2% solution): recent studies report antifungal properties against M. canis and Trichophyton spp.
- Advise that treatment can be both frustrating and expensive, especially in multi-animal households or with recurrent cases; consider referral to a veterinarian with expertise in treatment of dermatophytosis.
MEDICATIONS
DRUG(S) OF CHOICE
- Topical therapy and clipping—recommended concurrently with systemic therapy; may help prevent environmental contamination; may be associated with an initial exacerbation of signs
- Rinses: lime sulfur (1:16 dilution or 8 oz. per gallon of water), miconazole/chlorhexidine (0.2%), or enilconazole (0.2%) applied once to twice weekly; lime sulfur is odoriferous and can stain; enilconazole is not currently approved for use in companion animals in the US. Shampoos containing 1–2% ketoconazole, miconazole, or 0.5% climbazole; a minimum of a 3-minute contact time is recommended; have little to no residual effect.
- Use of an Elizabethan collar, particularly in cats, is recommended to prevent ingestion of these products.
- Griseofulvin—effective but use is declining due to relatively high costs and side effects.
- Ketoconazole—true efficacy unknown; some studies have shown in vitro resistance of M. canis: dogs, 10 mg/kg PO q24h or divided q12h for 4–8 weeks; anorexia and vomiting are the most common side effects; not recommended in cats.
- Itraconazole—similar to ketoconazole, but more effective; fewer side effects, expensive: dogs, 5–10 mg/kg PO q24h for 4–8 weeks; cats, 10 mg/kg PO q24h for 4–8 weeks or until cured. Alternate dosing—20 mg/kg q48h cats and dogs. In some cats, dosage regimen is altered after 4 weeks of therapy to every other week schedule for a total of 8–10 weeks of therapy; alternative schedule—one-week-on, one-week-off with apparent efficacy to reduce drug cost; manufactured drug preferred over compounded formulations due to absorption/concentration variability.
- Terbinafine—may be helpful in cases resistant to azole drugs; dogs, 20–30 mg/kg q12–24h for 4–8 weeks; cats, 20–40 mg/kg q24–48h for 4–8 weeks; dermatophyte carriers, 8.25 mg/kg q24h for 4–8 weeks; side effects may include gastrointestinal upset, hepatotoxicity, neutropenia, and pancytopenia.
CONTRAINDICATIONS
- Corticosteroids: can modulate inflammation and prolong the infection.
- Griseofulvin: cats with FeLV or FIV; teratogen.
PRECAUTIONS
- Ketoconazole
- Hepatopathy has been reported and can be severe in cats.
- Inhibits endogenous production of steroid hormones in dogs.
- Itraconazole
- Rare vasculitis and ulcerative skin lesions at doses of 5 mg/kg q12h; not noted in patients receiving 5 mg/kg q24h.
- Hepatotoxicity reported infrequently in dogs.
- Terbinafine
- Gastrointestinal upset, hepatotoxicity, and bone marrow suppression (pancytopenia, neutropenia). Decrease dosage with renal and/or hepatic insufficiency. Cimetidine increases blood concentration; rifampin decreases blood concentration.
- Lime-Sulfur Solution – Ingestion of lime sulfur may lead to oral erosions.
ALTERNATIVE DRUG(S)
- Lufenuron—a chitin synthesis inhibitor used in flea control; not effective in controlled studies.
- Fluconazole—effectiveness not well documented in studies; less expensive than itraconazole.
FOLLOW-UP
PATIENT MONITORING
- Dermatophyte culture is the only appropriate method for monitoring response to therapy; many animals clinically improve but remain culture-positive.
- Repeat fungal cultures toward the end of the treatment regimen and continue treatment until at least two subsequent cultures are negative.
- In resistant cases, cultures should be repeated weekly using the toothbrush technique.
- Weekly or biweekly CBC if treated with griseofulvin; periodic evaluation of liver enzymes if treated with ketoconazole, itraconazole, or terbinafine.
PREVENTION/AVOIDANCE
- Initiate a quarantine period and obtain dermatophyte cultures of all animals entering the household to prevent reinfection from inapparent carriers.
- Consider the possibility of rodents aiding in the spread of the disease.
- Decontaminate the environment.
- Avoid infective soil if a geophilic dermatophyte is cultured.
- Consider prophylactic treatment of exposed animals.
POSSIBLE COMPLICATIONS
False-negative dermatophyte culture
EXPECTED COURSE AND PROGNOSIS
Many animals will “self-clear” infection over a period of a few months.
Treatment hastens clinical cure and helps reduce environmental contamination.
Some infections, particularly in longhaired cats or multi animal situations, can be persistent.
MISCELLANEOUS
ZOONOTIC POTENTIAL
- Dermatophytosis is a significant zoonosis.
- Considered a low level pathogen; disease is not life-threatening, can be easily treated, but may cause scarring.
PREGNANCY/FERTILITY/BREEDING
- Griseofulvin is teratogenic.
- Ketoconazole can affect steroidal hormone synthesis, especially testosterone.
SYNONYMS
Ringworm
ABBREVIATIONS
FeLV = feline leukemia virus
FIV = feline immunodeficiency virus
H&E = hematoxylin and eosin
Visit your veterinarian as early recognition, diagnosis, and treatment are essential.
You may also visit – https://www.facebook.com/angkopparasahayop
